Publications IPH Magazine IPH Magazine, issue #14 Current Hospital Master Plan

- Current Hospital Master Plan
- Architecture Regulations for Healthcare Facilities in Brazil
- How Hospital Rooms Went from Airy Temples to "Inhuman" Machines
- The healthcare hub
- Santa Casa de Misericórdia de São Paulo: A hospital architectural heritage
- How Architecture Has Influenced the Promotion of Hospital Hotel Services and Humanization
Current Hospital Master Plan
Jonas Badermann de Lemos
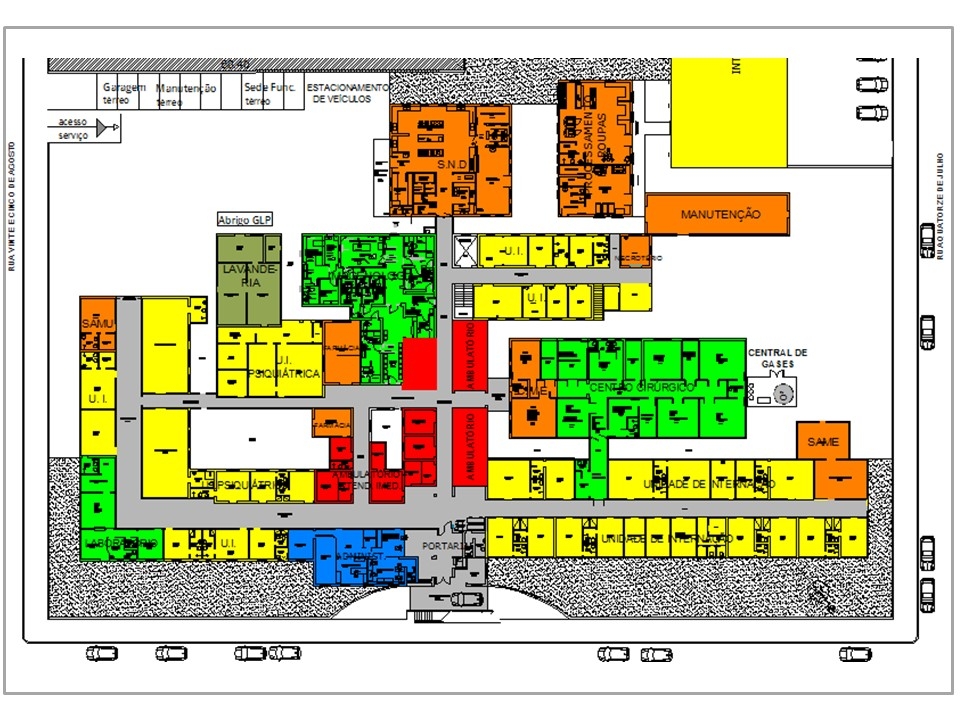 Picture 1 Case 1 Hospital Master Plan for an existing hospital Floor plan with the existing zoning of the functional unities. Source: Badermann Arquitetos, 2015.
Picture 1 Case 1 Hospital Master Plan for an existing hospital Floor plan with the existing zoning of the functional unities. Source: Badermann Arquitetos, 2015.

 Picture 3 Case 1 Hospital Master Plan for an existing hospital Graphic Summary concerning the Diagnosis and Prognosis. Source: Badermann Arquitetos, 2015.
Picture 3 Case 1 Hospital Master Plan for an existing hospital Graphic Summary concerning the Diagnosis and Prognosis. Source: Badermann Arquitetos, 2015.

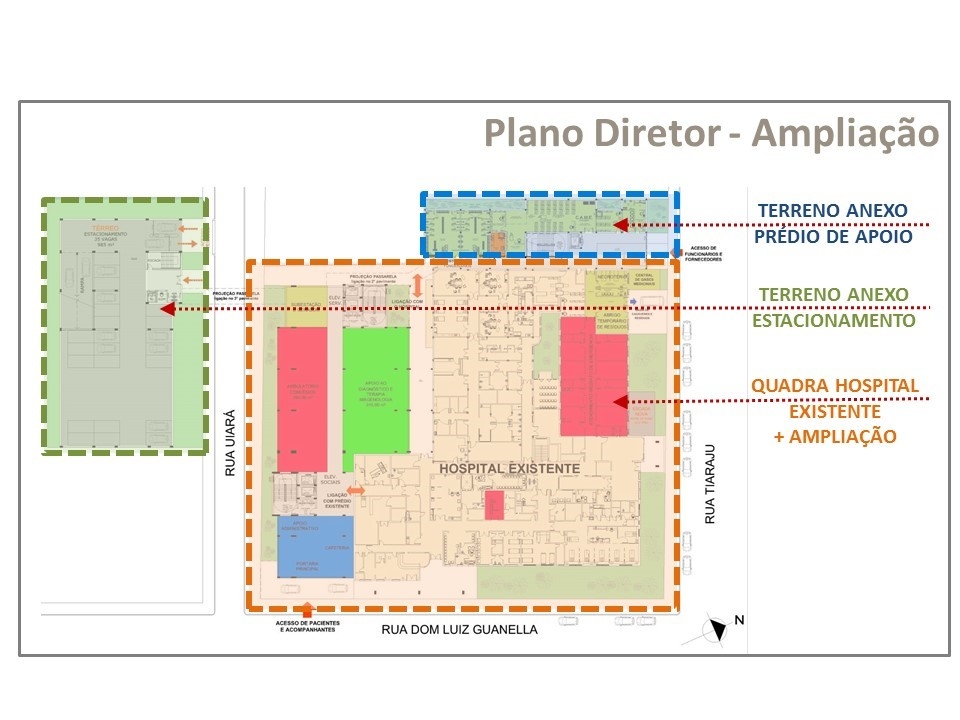




 Picture 7 Case 3 Hospital Master Plan for a new hospital Architectonic Project Constraints. Source: Badermann Arquitetos, 2016.
Picture 7 Case 3 Hospital Master Plan for a new hospital Architectonic Project Constraints. Source: Badermann Arquitetos, 2016.


 Picture 10 Case 3 Hospital Master Plan for a new hospital Architectonic Project Simplified Plan. Source: Badermann Arquitetos, 2016.
Picture 10 Case 3 Hospital Master Plan for a new hospital Architectonic Project Simplified Plan. Source: Badermann Arquitetos, 2016.
 Picture 11 Case 3 Hospital Master Plan for a new hospital Architectonic Project for Admission Unities. Source: Badermann Arquitetos, 2016.
Picture 11 Case 3 Hospital Master Plan for a new hospital Architectonic Project for Admission Unities. Source: Badermann Arquitetos, 2016.


A hospital is a building that accommodates a variety of functions, it is the most dynamic space of the contemporary society. Overseeing it represents a great challenge, considering the countless services and diversity of activities that are held there. Inside this building one may find a variety of facilities from a hotel, laboratory, laundry, pharmacy to even a restaurant. Such institution must have qualified administrative management and its healthcare services must respect strict protocols. Inside hospitals we find unique interpersonal relationships standards and continuing education takes place daily. There we can find a variety of treatments and a variety of patients, each one presenting a specific pathology going to the hospital searching for health, to keep it or recover it. Besides, in hospitals there are people from patients to those working there from the most diverse backgrounds, such as: doctors, nurses, managers, suppliers, pharmacists, general workers, maintenance technician, among others, which makes it hard to establish professional perspectives. Finally, a hospital deals with critical topics for the human being, among them: health, sickness, death, birth, fear, beliefs, altogether, it deals with psychological and subjective matters, i.e. the aspects that demand emotional self-control.
Over the last few years, hospitals have felt the need to adjust to the new type of customer. They have become more demanding with expectations equally more specific due to the increasing evolution of technology, higher levels of education and more access to information. The relationship between healthcare providers and patients reflects the new reality since the latter expects higher quality of services. Adding to that, the number of people with health insurance has skyrocketed over the last years, which has forced hospitals to rethink and expand their facilities.
This process of changing and modernization is clear in the Brazilian regulations, perceptible, among other aspects, in the evolution of hospital heterogeneity. By studying the Diagnosis and Therapy Care Services (Serviços de Apoio ao Diagnóstico e Terapia) that deals with outpatients and inpatients, for instance, we see a staggering increase. The Ordinance 400 from 6 December 1977, in chapter 5, which concerns the Diagnosis and Treatment Complimentary Services Unity, establishes few unities in comparison to the same group in the current regulation, emphasizing the lack of technology from four decades ago. In the case of imaging exams, the X-ray device was all the technology used at the time.
The unities described were as follows:
- Physical Therapy Unity;
- Hemotherapy Unity;
- Clinical Pathology Unity;
- Anatomical Pathology Unity;
- Clinical Radiology Unity;
- Electrocardiography Unity and
- Medications Dispensary.
We may also notice, in the 1977's regulation, the emphasis on the total built area of at least 45 m²/bed for general hospitals with up to 150 beds. Nowadays, the rule is to consider twice or even three times this area. Specifically, for the Diagnosis and Therapy Care Unity, the recommendation used to be 12 m²/bed. Nowadays, the area reserved for the services of this unity are not proportional to the number of beds, but to the caring nature of the organization, stretching to the commercial nature of the healthcare facility, surpassing, most of the time, the area recommended in the 1977s regulation that guided the architectonic design.
On 11 November 1994, the Ordinance 1884 was published. It added many other services to that comprehensive group of Diagnosis and Therapy Care Services. It was therefore proved the technological improvement and, consequently, the doors were open for the hospitals to embrace them. Besides the unities mentioned above, there was the establishment of the Imaging Unity, which included ultrasonography, MRI and radiology exams through the results of fluoroscopic or radiographic studies. They are obtained through cardiovascular radiology or tomography. Echocardiogram, ergometry, phonocardiogram and electroencephalogram exams were added to the list of exams expressed in graphic drawings. The activities concerning Nuclear Medicine, Radiotherapy, Chemotherapy and Dialysis were also included. The technological improvement of the Ordinance 1884 can also be proved by their decision to merge the Surgery Unity with the Therapy and Diagnosis Care Services. The evolution of surgical technics enabled the concept of ambulatory surgery, in which patients stay under observation for 12 to 24 hours and do not need to be admitted. Therefore, the ambulatory treatment was expanded with the help of all the several teams within the hospital and, consequently, other medical disciplines were included, inaugurating the concept of Partial Hospital Program. The hospitals, then, progressively received patients that were not admitted, they are called outpatient and stay for 24 hours maximum in the hospital and receive similar care to the ones admitted since they perform diagnostic and therapeutic procedures and receive infusions.
The Regulation RDC #50 from 21 February 2002, that replaced the Ordinance 1884, showed little improvement regarding the new technologies. From it, it is worth mention the inclusion of the hyperbaric oxygen therapy program.
Nowadays, when we compare the Brazilian regulation with the medical care technic used in hospitals and the use of new technologies, we become conscious of a misalignment the need of modernization. The regulation is not consistent with several procedures carried out, thus leading to a compulsory practice of an obsolete normative planning. Now that we are discussing the re-examination of the RDC 50, we must think about its character. What type of normative instrument should be established? One that is open to regular adaptations and transformations or one that rules activities, programs, areas and dimensions, cancelling out the architectonic correlation with new processes? An instrument that corresponds to the strategic planning and is flexible or the one that accords with the normative planning with strict rules that forbid developments? We cannot forget that the necessity program suffers constant alterations and processes are often evaluated. In the search of ultimate quality, architecture and facilities are rapidly changed. The complexity and functional aspect of a hospital demands a strategic planning supported by enduring discussion and analysis, whose focus is the appreciation of the patient and healthcare processes. We understand, therefore, that the work of hospital architecture assumes a professional training that goes beyond the simple formal and programmatic conception of a building, requiring an architect with specific, comprehensive, circumstantial and updated knowledge.
The use of technology in healthcare, considering the group perspective and medical, economic, social and ethical implications, is of great value for hospitals and causes a rupture in the traditional hospital model (SILVA, 2011). Healthcare work was no longer craft work once it made use of the technology available, thus reshaping the organization of healthcare work in its various professional connections that relate within the hospital. Consequently, the building must adapt to the new processes. There is the need for constant reviews and developments that are compatible with the humane and technological evolutions. Buildings must be progressively adapted to the: strategies of the institution, effortlessness of healthcare processes, operational costs, undemanding maintenance, water consumption and energy efficiency. Therefore, architecture assumes another perspective and begins to participate decisively in the healing process of patients, corresponding to the current results from the Evidence Based Design studies, which confirms the positive impact that elements such as natural ventilation, natural light exposure indoors, the view to outdoors areas and positive distractions have on patients and employees. Positive distractions are activities or events that the hospital organizes that inspire positive feelings in the patient, detracting their attention from their physical and emotional aspects through, for an example, music, art exhibitions, plays, social encounters, playing with pets, among others.
Gradually, hospitals have become centers of high technology with swaying functions, i.e. on one hand the functions that keep people healthy, through diagnosis and prevention treatments, and on the other, caring for critical patients that demand the most advanced technology to survive. At the same time, hospitals must be connected to the healthcare network of a location, region and country, acting as a reference guided by strategies of ultimate quality and developing permanent activities of investigation, process evaluation and feedback.
The hospital administration of nowadays presents some attributes that are different from the ones of the past, since hospitals are currently conceived as institutions that provide healthcare services and that are at the clients' permanent disposal and ready to perform in a world of competency and quality (MALAGÓN-LONDOÑO, 2000). Such competency must be based on: planning, organization, employee satisfaction, budget, management evaluation, feedback and ethics.
The strategic planning, therefore, acquires relevant importance: it consists of a process of devising and putting into effect organizational strategies to implement the organization and its mission in the environment where they are action. The strategic planning takes on a determinant role, since it represents a course of action chosen by the organization from the assumption that an anticipated and different position may represent gains and advantages regarding the present situation. Changing is a matter of survival for organizations. It is the process of strategic planning that is going to guide them towards the development and designing of actions that might assure their ongoing and sustainable evolution (CHIAVENATO; SAPIRO, 2010).
Strategic planning is the first step of the Master Planning. First, the purpose of the hospital must be clearly defined, since organizations have a raison dêtre, a goal, a mission, which is the operative synthesis of its natures and central values. The raison dêtre of a hospital is its commitment with the society in five topics: what it is done, why it is done, where it is done, for whom it is done and how it is done. Unfortunately, this is not what we can usually observe in healthcare institutions. The solution for specific problems prevail, overloading the system with unsuitable answers that, most of the time, compromise the functionality of the. We can often observe this situation in inappropriate employment relationships between the unities and a temporary organization, triggering an unorganized growth that did not had a systemic vision of planning. The Hospital Master Planning, therefore, it is essential when planning an organization and it is imperative during two stages: at first, to reorganize the physical and functional aspects of an existing hospital, and, secondly, to conceive the architect project of a new hospital.
During both stages, the physical and functional architectonic planning is needed to guide the evolution of the work through a methodology that may be applied in both situations.
In an existing hospital, the information system allows to rapidly get acquainted with administrative and medical care activities. This collection of data makes it possible to identify the epidemiologic environment in which the organization is, thus helping to eventually change course of action that will be proposed in the Master Planning, which will be responsible for defining the types of intervention to be carried out based on the improvement of existing capacity, the situation of the infrastructure and on the estimation for service demands. Moreover, the Master Planning will be accountable for the remodeling and potential expansions of the building using required qualifications, always prioritizing scaling down risks.
Designing a Hospital Master Planning in an existing organization Stages and Goals
| Stage | Equivalence | Goals |
| I. Analysis | Strategic Planning | To understand the purpose of the hospital and the strategies related to social and commercial interests. |
| Locoregional Epidemiology | To study patients and their cultural and socioeconomic aspects, morbid tendencies, demography, births and deaths. To study the estimation for the population and the ageing rates. To understand the situation of reference and counter-reference of patients. | |
| Locoregional healthcare structure | To study the healthcare network (basic, ambulatorial and hospital medical care), number of facilities, number of specialized professionals, equipment and financing. To observe future Technologies that could be added to the services. | |
| Public perception of the organization | Understand what is the perception that patients, clients and employees have of the organization. | |
| Infrastructure | To verify the maintenance of the building infrastructure, considering electric wiring, hydraulic and sewer systems, firefighting system, climatization, dispensing hood, medical gases, energetic efficiency, sewage system, among others. | |
| Architectonic aspects | To analyze the functional, social and cultural aspects of the building, considering accessibility, contiguity between unities/services and their functional relationships, circulatory organization, outdoor access, control and reception, distribution of meals and supplies, flexibility, buildings useful life and matters concerning humanization. To exam the process of the activities that guide the architectonic plan. | |
| II. Diagnosis | Development of the Architectonic and Infrastructure Diagnosis Report | To verify if the healthcare and commercial purposes are accomplished by the architectonic plan. To compare the required regulation concerning physical and functional aspects to the current situation. To list conflicts. To provide an infrastructure diagnosis. |
| III. Prognosis | Development of the Functional Plan | To establish which are the required services to run a hospital and which should be included to the program of needs by projecting the demand according to the strategic planning. To verify the management style of healthcare facilities and the number of employees. To ascertain the assignments and list of activities for the healthcare facility according to the RDC # 50 and the processes carried out. To develop the Program of Needs and department board. To verify the Program for Biomedical Equipment and its spatial, installation and energetic consumption aspects. |
| IV. Hospital Master Planning | Designing the Hospital Master Plan | To sum up the Functional Plan into a Prognostic Report and use it for the architectonic solution for the organization through schematic two-dimensional or three-dimensional plans. To propose a new zoning, if necessary, considering the land, the access, the interdepartmental relationships, the circulatory organization and the energetic efficiency. To indicate the possibility of future expansions. To represent the final architectonic solution. |
We may observe from the above table the introduction of an internationally known concept: Hospital Master Planning, which is the synthesis of all the requirements for a hospital to operate not only architectonic aspects, but also the ones concerning the institution, management and the building infrastructure.
 Picture 1 Case 1 Hospital Master Plan for an existing hospital Floor plan with the existing zoning of the functional unities. Source: Badermann Arquitetos, 2015.
Picture 1 Case 1 Hospital Master Plan for an existing hospital Floor plan with the existing zoning of the functional unities. Source: Badermann Arquitetos, 2015.
Picture 2 Case 1 Hospital Master Plan for an existing hospital Summary of the Diagnosis / Prognosis. Source: Badermann Arquitetos, 2015.
 Picture 3 Case 1 Hospital Master Plan for an existing hospital Graphic Summary concerning the Diagnosis and Prognosis. Source: Badermann Arquitetos, 2015.
Picture 3 Case 1 Hospital Master Plan for an existing hospital Graphic Summary concerning the Diagnosis and Prognosis. Source: Badermann Arquitetos, 2015.
Picture 4 Case 2 Hospital Master Plan for an existing hospital - Summary of the Diagnosis / Prognosis. Source: Badermann Arquitetos, 2016.

Picture 5 Case 2 Hospital Master Plan for an existing hospital Master Plan - Expansions. Source: Badermann Arquitetos, 2016.




Picture 6 Case 2 Hospital Master Plan for an existing hospital Schematic Volumetric Perspectives. Source: Badermann Arquitetos, 2016.
The beginning of project for a new hospital demands more cautious. Therefore, the necessary data that will guide the Hospital Master Planning must be previously collected, systematically analyzed and studied. The project must consider the land and its geographic and environmental surroundings, the population, the healthcare network, the local services and the demand for new services.
Designing a Hospital Master Planning for a new institution Stages and Goals
| Stage | Equivalence | Goals |
| I. Analisis | Strategic Planning | To envision the mission of the hospital and the strategies concerning social and commercial interests. |
| Locoregional Epidemiology | To study patients and their historical evolution. Their cultural and socioeconomic aspects, morbid tendencies, demography, births and deaths. To study the estimation for the population and the ageing rates. To understand the situation of reference and counter-reference of patients. | |
| Locoregional healthcare structure | To study the healthcare network (basic, ambulatorial and hospital medical care), number of facilities, number of specialized professionals, equipment and financing. To observe technologies that are needed and the ones that could be added to the services in the future. | |
| II. Prognosis | Development of the Functional Plan | To establish which are the required services to run a hospital and which should be included to the program of needs by projecting the demand according to the strategic planning. To verify the management style of healthcare facilities and the number of employees. To ascertain the assignments and list of activities for the healthcare facility according to the RDC # 50 and the processes carried out. To develop the Program of Needs and department board. To verify the Program for Biomedical Equipment and its spatial, installation and energetic consumption aspects. To contemplate the infrastructure and the standard for energetic efficiency. |
| III. Hospital Master Planning | Designing the Hospital Master Plan | To sum up the Functional Plan and use it for the architectonic solution for the organization through schematic two-dimensional or three-dimensional plans. To propose the zoning, considering an efficient architectural project the land, the access, the interdepartmental relationships, the circulatory organization and the energetic efficiency. To indicate the possibility of future expansions. To represent the final architectonic solution. |
 Picture 7 Case 3 Hospital Master Plan for a new hospital Architectonic Project Constraints. Source: Badermann Arquitetos, 2016.
Picture 7 Case 3 Hospital Master Plan for a new hospital Architectonic Project Constraints. Source: Badermann Arquitetos, 2016.
Picture 8 Case 03 Hospital Master Plan for a new hospital Architectonic Project Accesses. Source: Badermann Arquitetos, 2016.

Picture 9 Case 3 Hospital Master Plan for a new hospital Architectonic Project Volumetric Perspective. Source: Badermann Arquitetos, 2016.
 Picture 10 Case 3 Hospital Master Plan for a new hospital Architectonic Project Simplified Plan. Source: Badermann Arquitetos, 2016.
Picture 10 Case 3 Hospital Master Plan for a new hospital Architectonic Project Simplified Plan. Source: Badermann Arquitetos, 2016. Picture 11 Case 3 Hospital Master Plan for a new hospital Architectonic Project for Admission Unities. Source: Badermann Arquitetos, 2016.
Picture 11 Case 3 Hospital Master Plan for a new hospital Architectonic Project for Admission Unities. Source: Badermann Arquitetos, 2016.

Picture 12 Case 3 Hospital Master Plan for a new hospital Implementation in stages. Source: Badermann Arquitetos, 2016.
The architectonic project that results from the Master Planning is determinant for the efficiency of hospital management. It is recommended to minimize the distances that patients, employees and suppliers may go through, considering the functional relations and the connection among unities. Hospitals expand and change. Therefore, when deciding on and envisioning an architectonic project, it is fundamental to establish an efficient circulatory organization for the intramural flux of people and to think about a rational structural system, besides setting aside free areas for further expansions. A rational structural system is a network that allows services to be altered without the interference of beams and pillars. When estimating the program of needs and when suggesting the plan, despite the uncertainties of the future, it is important to consider a demand for, at least, ten years.
Nowadays, when we think about hospitals, we do not picture just a group of doctors and nurses gathering around the infirmary. We think about highly organized institutions that, besides recovering the physical conditions of patients, encourage coordinated actions to keep and preserve health. We think about centers that use high technology to diagnose and treat several pathologies, where there is the practice of teaching and continuing education is encouraged daily among the institutions professionals. We think about a place where the administration is relevant to manage and control several concentrated and autonomous activities. We think about the infrastructure available to hold the high technology of equipment, as well as to train the professionals responsible for it. This conception makes us realize that the spatial organization of a hospital is not a simple task and that implies a multiplicity of data, which cannot be obtained unless the various specialized professionals get involved. The Master Planning, therefore, to meet general expectations, must have a multidisciplinary formulation, since it is not just a compilation of architectonic concepts, but also includes administrative, healthcare and infrastructure aspects, among others. As a result, we propose assembling a task force with representatives from the general departments of the hospital, such as: target activities, patient management, administration, technical and logistic support, and, when necessary, teaching and specialized advisors.
The hospital has the moral responsibility to provide services of high standards, hence the need to purpose efficient planning strategies that include the Hospital Master Planning, which will guide the architectonic path for the institution, the stages of the construction, modernization of infrastructure and financing in accordance with the political and administrative decisions.
A thoughtful and well-conceived Hospital Master Planning will guarantee a harmonious environment for the hospital, both physically and functionally.
Bibliography
ALATRISTA, Celso Bambarén; BAMBARÉN, Socorro Alatrista Gutiérrez de.Programa médico arquitectónico para el diseño de
hospitales seguros. 1ª ed. Lima: SINCO editores, 2008.
BADERMANN DE LEMOS, Jonas. Planos Diretores para Estabelecimentos Assistenciais de Saúde. In: BITENCOURT, Fabio; COSTEIRA, Elza (org.). Arquitetura e Engenharia Hospitalar. Rio de Janeiro: Rio Books, 2014.
BRASIL. Ministério da Saúde. Secretaria Nacional de Ações Básicas de Saúde. Divisão Nacional de Organização de Serviços de Saúde. Portaria nº 400 de 6 de dezembro de 1977: Normas e Padrões de Construções e Instalações de Serviços de Saúde. Brasília, 1977.
BRASIL. Ministério da Saúde. Secretaria de Assistência à Saúde. Departamento de Normas Técnicas. Portaria nº 1884 / GM de 11 de novembro de 1994: Normas para Projetos Físicos de Estabelecimentos Assistenciais de Saúde. Brasília, 1994.
BRASIL. Agência Nacional de Vigilância Sanitária (ANVISA). Resolução RDC nº 50 de 21 de fevereiro de 2002: Dispõe sobre o Regulamento Técnico para planejamento, programação, elaboração e avaliação de projetos físicos de estabelecimentos assistenciais de saúde. Brasília, 2002.
CHIAVENATO, Idalberto; SAPIRO, Arão. Planejamento Estratégico. Fundamentos e Aplicações. Da intenção aos resultados. 2ª ed. Rio de Janeiro: Editora Elsevier, 2010.
MALAGÓN-LONDOÑO, Gustavo. Generalidades sobre Administração Hospitalar. In: MALAGÓN-LONDOÑO, Gustavo; MORERA, Ricardo Galán; LAVERDE, Gabriel Pontón (org.). Administração Hospitalar. 2ª ed. Rio de Janeiro: Editora Guanabara Koogan S.A., 2003.
SILVA, Alceu Alves da. Cenários e Tendências em Saúde. In: ALLGAYER, Cláudio. Org. Gestão e saúde: temas contemporâneos abordados por especialistas do setor. Porto Alegre: Instituto de Administração Hospitalar e Ciências da Saúde, 2011.
VECINA NETO, Gonçalo; MALIK, Ana Maria. Org. Gestão em Saúde. Rio de Janeiro: Editora Guanabara Koogan Ltda, 2011.
Send by e-mail:


